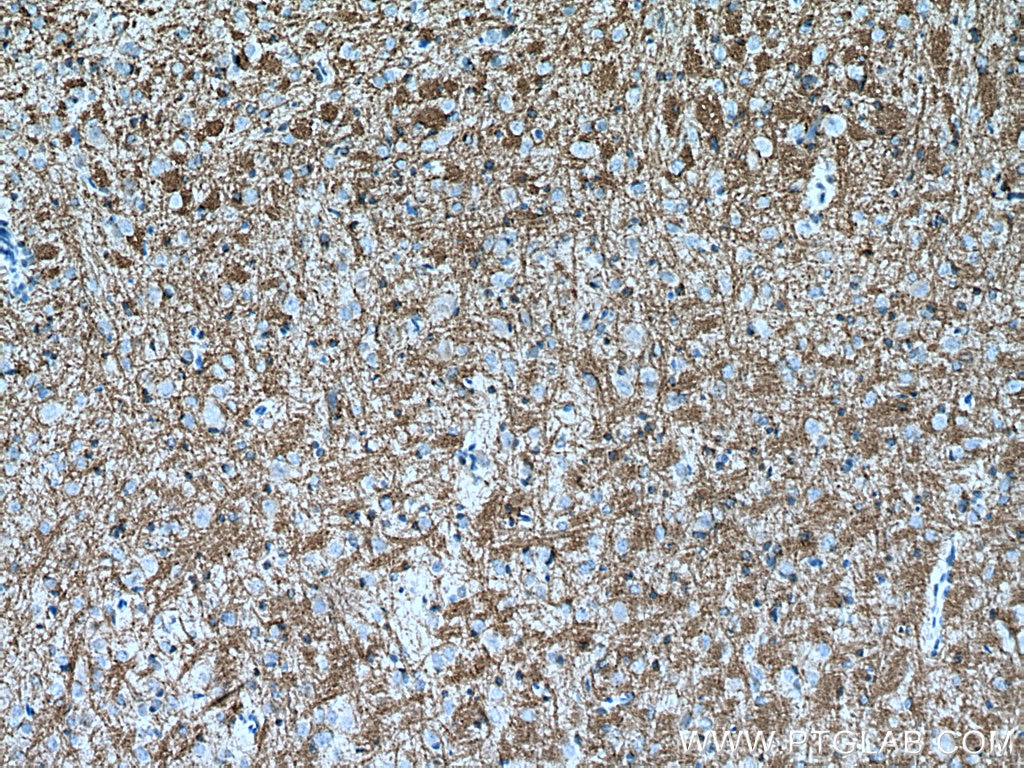
Upon telephone consultation after 2 months (day 63), he reported he felt well and was back to work in shifts, with no residual symptoms, no restrictions, and no medication. The serum MOG antibody titre was reduced to 1:320, while further laboratory tests including mGluR1 antibody were normal. Follow-up MRI showed a resolution of signal alterations (Fig. Extensive follow-up neuropsychological assessment was entirely normal, with above average results in all dimensions (Table 1). There was no headache, no focal neurological deficits, and no meningism. At a follow-up visit (day 35), the patient felt well. He was discharged home and gradually resumed work. 
The patient’s general condition and headache improved gradually after completing the treatment, corresponding to marked improvement in the brain MRI on day 17 (Fig. One thousand milligrams methylprednisolone i.v. Dexamethasone and aciclovir were discontinued. 2), and a low metabotropic glutamate receptor 1 (mGluR1) antibody titre (fixed cell assay, 1:40 see also Table 2). Serum and CSF studies revealed a serum myelin oligodendrocyte glycoprotein (MOG) antibody titre of 1:640 (live-cell assay, see Fig. SARS-CoV-2 and HSV 1, 2 PCR in the CSF were negative, as was serology for Lyme borreliosis and HIV. There was no intrathecal IgG synthesis An extensive search for infectious, paraneoplastic, and autoimmune causes of encephalitis was performed. CSF analysis revealed a pleocytosis with 31 cells per μl (normal range, nr, < 5). 
Comprehensive neuropsychological assessment on day 16 showed no memory impairment, but mild impairment in executive functions (Table 1). Brain MRI (day 11) showed multiple disseminated pathological T2 and FLAIR hyperintensities, predominantly cortically, without any contrast enhancement (Fig. Blood laboratory tests were unremarkable. Further neurological examination was normal. On physical examination at admission, he was fully oriented and had some neck rigidity. He had been started on ASS, low-dose heparin, dexamethasone and aciclovir. He reported fever, neck stiffness, general weakness and a loss of smell and taste. Ten days later, he was admitted to our hospital because of severe headache (verbal rating scale, VRS 8/10) that had started a week previously, few days after his positive test. This case highlights a possible association between inflammation due to COVID-19 and transient secondary autoimmunity with transient MOG antibodies and atypical clinical presentation.Ī previously healthy and asymptomatic 22-year-old male police officer was confirmed SARS-CoV-2 positive by PCR testing while in contact quarantine at home (= day 0). ConclusionsĬovid-19 manifestations in the CNS include encephalitis with variable course and prognosis. The patient made a full recovery, with no signs of deterioration over the following months. Consequently, the MOG antibody titer decreased and MRI lesions were resolving. The headache improved with analgetic treatment and i.v. 
Further laboratory examination revealed a serum MOG antibody titre. Brain MRI and cerebrospinal fluid (CSF) analysis were suggestive for encephalitis. Neuropsychological testing revealed distinct executive deficits. Case presentationĪ 22-year-old male, with PCR confirmed Covid-19 infection was admitted because of persistent headache. Here, we describe a unique case of a young man with Covid-19 and transient MOG-positive encephalitis, with a benign course. While Covid-19 predominantly affects the respiratory system, neurological manifestations including encephalitis occur in some patients, possibly affecting the course and outcome of the disease.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
